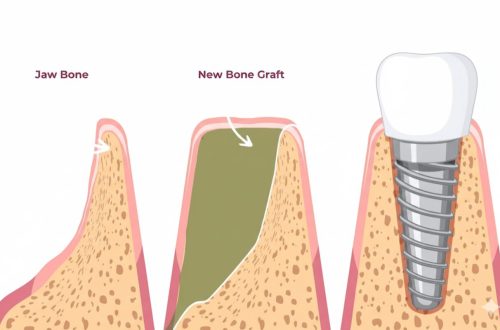
Losing a single tooth may seem like a small problem, but its impact reaches far beyond appearance. Even one missing tooth can disrupt chewing efficiency, alter speech, and cause progressive changes in the jawbone. Research shows that the bone in an untreated extraction site can lose up to 25% of its volume within the first year, with continued resorption over time if no root or implant is present to stimulate the bone (Atwood, 1979; Schropp et al., 2003).
The most common reasons for single tooth loss include trauma, advanced tooth decay, and periodontal disease, all of which can compromise not only the lost tooth but also the long‑term stability of the surrounding teeth. When a gap remains in the dental arch, adjacent teeth tend to shift into the empty space, creating misalignment, bite problems, and increased risk of further tooth loss.
Addressing the problem early is critical. Replacing a missing tooth before significant bone loss occurs can simplify treatment, reduce the need for grafting procedures, and improve long‑term outcomes. This is where single dental implants stand out as the gold standard of care. Unlike traditional bridges that rely on grinding down healthy neighboring teeth, an implant functions as an independent, artificial root that preserves the surrounding bone and provides excellent long‑term stability.
Because of their ability to mimic natural tooth function and prevent further oral deterioration, single implants are recognized in modern restorative dentistry as the most biologically sound and durable solution for replacing a missing tooth.
What Is a Single Dental Implant?
A single dental implant is a fixed tooth-replacement option used to restore one missing tooth with one implant fixture placed in the jawbone and one prosthetic crown attached on top. It acts as an artificial tooth root and supports a custom-made crown that mimics the function and appearance of a natural tooth (Jung et al., 2012).
A complete single-implant restoration consists of three components:
- Implant fixture – surgically inserted titanium or zirconia root replacement
- Abutment – connector linking the implant and the crown
- Crown – the visible part that restores chewing and aesthetics
How it differs from other options:
| Feature | Single Dental Implant | Dental Bridge | Removable Partial Denture |
|---|---|---|---|
| Support | Implant anchored in bone | Uses adjacent teeth for support | Rests on gums/teeth, removable |
| Tooth preparation required | No | Yes – adjacent teeth must be prepared | No preparation, but less stable |
| Bone preservation | Yes – maintains jawbone through functional loading | No | Minimal to none |
| Stability | Fixed, high stability | Fixed, good stability | Lower stability, possible movement |
Key benefits:
- Bone preservation through mechanical stimulation that prevents resorption
- High functional stability for chewing and speech
- Long-term survival and predictability (10+ years documented success)
- No alteration of healthy neighbouring teeth
- Natural aesthetics and comfort
Who Is a Good Candidate for a Single Implant?
A good candidate for a single dental implant is generally a patient with adequate systemic health, sufficient bone density and volume at the missing tooth site, and good oral hygiene practices that support long-term implant maintenance. Candidates should be able to undergo minor oral surgery and commit to postoperative care to ensure proper healing and osseointegration (Esposito et al., 2012).
Key suitability factors:
- Good overall health, no active oral infections
- Adequate bone quantity for stable implant placement
- Healthy gums and effective daily oral hygiene
- Non-smoker or willing to reduce/stop smoking during healing
Possible contraindications where implant therapy may be limited or postponed include:
- Uncontrolled diabetes
- Smoking, especially heavy smoking due to impaired healing
- Insufficient bone volume requiring augmentation
- Severe periodontitis not yet treated
- Conditions affecting bone metabolism, radiation in the jaw area
Required diagnostics typically include:
- CBCT scan to evaluate bone volume, density, and anatomical structures
- Intraoral or panoramic X-rays for initial assessment
- Medical and dental history review, including medications and systemic risk factors
Step-by-Step Process of Getting a Single Implant
Diagnostic Phase
The treatment process begins with a comprehensive clinical consultation, including a review of medical history and oral health status. A CBCT scan and intraoral evaluation are performed to assess bone volume, density, and proximity to anatomical structures. Digital planning and 3D analysis are used to determine optimal implant positioning, angulation, and prosthetic requirements to ensure long-term function and aesthetics.
Surgical Placement
Under local anesthesia, the clinician prepares the osteotomy site using sequential drilling protocols. The implant fixture is placed with controlled torque—commonly in the range of 35–45 Ncm—to ensure sufficient primary stability, which is critical for predictable osseointegration. The surgical site is then closed or fitted with a healing component, depending on the loading strategy.
Healing Phase (Osseointegration)
A healing period of approximately 8–16 weeks is required, depending on bone quality, anatomical location, and systemic factors. During this stage, new bone forms directly on and around the implant surface, establishing secondary (biological) stability. The patient must avoid excessive mechanical loading or movement at the site to reduce the risk of fibrous encapsulation and implant failure.
Abutment and Crown Placement
After successful osseointegration, the implant is uncovered (if submerged), and a prosthetic abutment is connected. Soft tissue contours stabilize around the abutment, after which the custom crown is fabricated and precisely fitted. Final adjustments are made to ensure proper occlusion, function, and aesthetics.
Advantages and Disadvantages of Single Implants
Advantages:
- No need to alter adjacent teeth: A single implant is self-supporting and does not require grinding down healthy neighboring teeth, unlike traditional bridges [Pjetursson et al., 2007].
- Preserves bone: By transferring chewing forces directly into the jawbone, implants help prevent bone resorption that typically follows tooth loss [Buser et al., 2017].
- Long-term stability: With proper care, single implants show high long-term survival rates exceeding 95% over ten or more years.
- Natural function and look: Implants restore near-complete masticatory efficiency and are customized for aesthetic integration with natural dentition.
Disadvantages:
- Higher cost: Implant treatment is generally more expensive upfront compared to bridges or removable prosthetics.
- Requires minor surgery: The procedure involves surgical placement, which carries typical surgical risks and may be intimidating for some patients.
- Longer treatment time than a bridge: Healing and osseointegration extend the timeline, often requiring several months before the final crown is placed.
Risks and Possible Complications
While single dental implants are generally safe and predictable, certain risks and complications may occur:
- Infection or inflammation (peri-implantitis): This is a bacterial infection affecting the soft and hard tissues surrounding the implant, often due to poor oral hygiene or pre-existing periodontal disease. It can lead to progressive bone loss if untreated.
(Renvert S, Quirynen M. “Risk indicators for peri-implantitis: a narrative review.” Clin Oral Implants Res. 2015) - Failure to integrate with bone: Known as failed osseointegration, this occurs when the implant does not fuse with the jawbone, often due to smoking, poor bone quality, or early loading.
- Prosthetic issues: These include complications such as a loose abutment screw, chipped or fractured crown, or occlusal misalignment. Though typically minor, they may require repair or adjustment. (Goodacre CJ et al., “Clinical complications with implants and implant prostheses.” J Prosthet Dent. 2003)
- Implant overload or bone loss over time: Excessive mechanical forces or bruxism can lead to bone resorption and implant failure, especially if occlusion is not properly managed.
Aftercare and Maintenance
Proper care after implant placement is essential to ensure long-term success. Daily oral hygiene plays a crucial role—patients should brush at least twice a day and use interdental brushes or floss to clean around the implant site and under the crown. Specialized implant floss or soft picks can also help remove plaque without damaging surrounding tissue.
Smoking should be avoided entirely, as it significantly increases the risk of peri-implant diseases and impairs healing. Clinical studies consistently show that smokers have a higher rate of implant failure and complications.
In addition to home care, professional cleanings and check-ups every 6 months (or as advised) are critical. Dental professionals can monitor bone levels, check the fit of the prosthetic components, and identify early signs of inflammation or bone loss.
Consistent supportive implant therapy—both at home and professionally—significantly improves long-term outcomes and reduces the risk of peri-implant complications.
Cost Breakdown: What You’re Really Paying For
A single implant isn’t one item on a price list – it’s a bundle of several components and clinical steps. When you compare quotes between countries or clinics, always check whether these elements are included:
- Implant fixture – the titanium or zirconia screw placed in the jaw
- Abutment – connector between implant and crown
- Crown – the visible tooth (zirconia, ceramic, or PFM)
- Diagnostics – exam, panoramic X-ray and/or CBCT
- Surgical time & materials – anesthesia, sterile field, sutures, possible surgical guide
- Additional procedures (if needed) – extractions, bone graft, sinus lift, soft-tissue graft
- Follow-ups – post-op checks, suture removal, minor adjustments
Many “from €X” ads cover only the implant fixture, not the full implant-abutment-crown package.
Typical Price Ranges by Region (Single Implant + Crown)
Below are example ranges for one implant with abutment and crown, based on real clinic and comparison sites. Numbers are indicative, not fixed fees.
- USA – about $3,000–$6,000 for implant + abutment + crown in private practices.
Example: a US implant center lists $3,000–$6,000 per single implant including crown. Dental Specialists & Implant Center - UK – roughly £2,400–£4,500 per tooth in private clinics, including implant, abutment and porcelain crown. bupa.co.uk
- Germany – around €1,850–€2,400+ for a single implant with crown in German practices, depending on lab and materials. implantate.com
- Turkey – about €350–€600 for a single implant (often per implant fixture), with full packages for implant + crown still far below Western prices. NewHolidays.co.uk
- Albania – very low package pricing; one comparison site lists a single titanium implant incl. abutment and crown at about $383, including consultation, 3D scans and surgery. Medical Tourism Co
What’s Usually Not Included
These items are often not part of a basic implant quote, or they may be billed separately:
- Extensive bone grafting or sinus lift procedures
- Sedation (IV sedation or general anesthesia)
- Temporary restorations (temporary crowns or provisional bridges)
- Post-operative medication and additional care if complications occur
- For dental tourism: flights, hotel accommodation, local transfers, unless clearly stated in a treatment package
Implant vs. Traditional Bridge: Comparison Table
| Feature | Single Dental Implant | Traditional Dental Bridge |
|---|---|---|
| Bone preservation | ✅ Yes – helps prevent bone loss | ❌ No – does not stimulate bone |
| Involves adjacent teeth | ❌ No – does not require altering neighboring teeth | ✅ Yes – requires reducing/reshaping healthy teeth |
| Longevity | 10–20+ years (often longer with proper care) | 7–15 years on average |
| Oral hygiene | Easier cleaning (similar to a natural tooth) | Harder (requires cleaning under the bridge) |
| Total cost | Higher upfront cost | Lower initial cost, but may require more replacements over time |
Conclusion: When Is a Single Implant the Best Choice?
A single dental implant is often the best choice for patients who want a permanent, stable, and natural-looking replacement for a missing tooth. It is especially suitable when the adjacent teeth are healthy and should not be reshaped or used as support for a bridge. Because an implant stimulates the jawbone, it also helps prevent long-term complications such as bone loss, changes in bite, and facial structure collapse.
While implants typically require a higher initial investment than traditional bridges or removable partial dentures, they provide superior long-term function, aesthetics, and oral health benefits. For patients who value a long-lasting solution that looks and feels like a natural tooth, a single implant is often the most predictable and clinically sound treatment option.
FAQ: Single Dental Implant
1) Does it hurt to get a single dental implant?
Most patients report mild to moderate discomfort for a short period after surgery. The procedure is typically performed under local anesthesia, so you should not feel pain during placement. Post-operative soreness is common for 1–3 days and may be managed with prescribed or OTC pain medication.
2) How long does a single implant take from start to finish?
The total timeline generally ranges between 3–6 months, depending on healing and bone condition. The treatment includes:
- Consultation + CBCT diagnostics
- Surgical placement
- Osseointegration (≈ 8–16 weeks)
- Abutment + crown placement
If bone grafting is needed, the process may take longer.
3) Is a single dental implant better than a bridge?
For most patients with healthy adjacent teeth, yes. A single implant does not require altering neighboring teeth and helps preserve jawbone volume through functional stimulation. Bridges may be faster and sometimes cheaper upfront, but they do not prevent bone loss and rely on grinding down healthy tooth structure.
4) What happens if I don’t replace a missing tooth?
Not replacing a missing tooth can lead to progressive bone resorption, shifting or over-eruption of nearby teeth, bite changes, difficulty chewing, and reduced facial support over time.
5) Can I eat normally with a single implant?
Yes, once fully healed. After the crown is placed and osseointegration is complete, patients typically regain chewing function close to natural teeth. However, in the early healing phase, a soft diet is required to avoid excessive force on the implant.
6) How long does a single implant last?
A well-maintained implant can last 15–20 years or longer, and many exceed 25+ years. Longevity depends on oral hygiene, bone health, systemic factors, and lifestyle habits such as smoking.
7) What material is better: titanium or zirconia?
Titanium implants are currently the most used and have the longest clinical success record. Zirconia implants are metal-free and preferred by patients seeking alternative or holistic options, but have fewer long-term studies.
8) Will people notice I have an implant?
Usually no. A custom ceramic or zirconia crown is designed to match the color, shape, and translucency of surrounding teeth, making the implant indistinguishable from natural dentition.
9) Are single implants safe for diabetics?
Well-controlled diabetics can successfully receive implants. Poorly controlled diabetes may increase complication and implant-failure risk due to impaired healing.
Source: American Diabetes Association – Dental Implants and Diabetes
https://diabetes.org/health/dental-care
10) Can smokers get single implants?
Yes, but smoking increases risk of implant failure, peri-implantitis, and delayed healing. Many surgeons recommend quitting smoking 2–4 weeks before and after surgery.